 Astonishingly, there are at least 34 million Americans that currently wear contact lenses regardless of their ocular condition. From presbyopia to astigmatism, lens technology has evolved to address the needs of a wide range of patients with varying ocular issues. However, the contact lens dropout rate remains a persistent concern for practices, especially with patients suffering from dry eye.
Astonishingly, there are at least 34 million Americans that currently wear contact lenses regardless of their ocular condition. From presbyopia to astigmatism, lens technology has evolved to address the needs of a wide range of patients with varying ocular issues. However, the contact lens dropout rate remains a persistent concern for practices, especially with patients suffering from dry eye.
A recent study found that 52.7% of contact lens wearers, compared to an estimated 14% to 33% of the general population, suffer from dry eye.1 In a 2010 global survey conducted by John Rumpakis, O.D., M.B.A., the primary reason patients discontinue use of their lenses is discomfort associated with dry eye (50%), followed by a preference for glasses (15.9%) and finally, expense (12.3%).2 As eye care practitioners, we struggle to work with financial constraints and our patients’ personal preferences. However, we can take steps to prevent a contact lens user from discontinuing use solely due to dry eye.
In this column, we’ll look at the patient profile of a contact lens user with dry eye, describe ways to screen for the disease and examine the many treatment options currently available.
The Dry Eye Dilemma
Dry eye is both a medical concern as well as a refractive issue, and should be treated before the initial prescription and/or continuation of lenses. By treating the eye first, you can then focus on equipping your patient with the most appropriate lens choice.
Ocular dryness and the use of contact lenses presents a considerable challenge: Contact lenses may exacerbate pre-existing dry eye, and can also induce dry eye in patients who may have previously never had any symptoms. This type of dry eye is a condition known as contact lens-induced dry eye (CLIDE). When a contact lens is placed on the pre-corneal tear film, the normal tear film is disrupted, which leads to more rapid tear film break-up and evaporation.3 Contact lens wear also can decrease corneal sensitivity and disrupt the normal tear secretion that is needed to preserve the ocular surface.4
Keep in mind that losing contact lens patients can significantly impact your practice’s income. In fact, each contact lens dropout costs an optometric practice an average of $21,695 over the lifetime value of that patient.2 These losses can be avoided if a patient’s dry eye is appropriately managed first.
Recognize Patient Behavior
It should be noted that a comprehensive dry eye exam is different from a regular check-up of a patient’s overall ocular health.
Before fitting your patient in contact lenses, conduct a thorough eye exam. Ask basic questions, such as whether your patient is experiencing any common signs of dry eye, including burning, stinging or grittiness. Upon clinical presentation, it is important to clearly differentiate between symptoms related to lid disease (blepharitis or meibomian gland dysfunction) and symptoms of allergy. For example, an allergic eye itches, while a dry eye burns and produces a gritty sensation.
Next, follow up with more detailed questions to gain some insight into your patient’s daily habits. Note non-compliant tendencies among your patients, such as sleeping in lenses or skipping cleaning regimens. Learn about your patient’s individual lens needs, such as how many hours of continuous lens wear is expected, to establish the most customized approach to their lens care. Consider switching your patient to a daily disposable lens, which may help alleviate many symptoms and improve compliance.
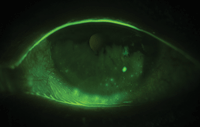
Diagnostic tests like staining reveal a dry eye patient’s symptoms such as increased tear film break-up. Being fully aware of your patient’s dry eye is crucial before outfitting them in lenses.
While collecting a personal history, find out about your patient’s home and work environments. Symptoms of ocular discomfort are higher among contact lens users who spend significant time in areas controlled by air conditioners and/or heating units, and those who are exposed to windborne and airborne pollutants.5
Visually taxing activities, such as reading, watching television or using a computer, can exacerbate dry eye symptoms.3 Suggest that your patients avoid these stressors for an extended period of time. These subtle changes in lifestyle can often have a significant impact on dry eye patients’ quality of life.
Finally, find out at what time of the day the symptoms are at their worst. Studies have shown that subjects with dry eye display impaired visual function in the evening rather than in the morning.6
Clinical Examination
There are several techniques used to diagnose dry eye.
• Fluorescein and lissamine green staining. These tests are used to evaluate the cornea, conjunctiva and tear film to get a clear picture of the extent of dry eye damage.
• Standard slit lamp. A physical examination is also needed to look for classic signs of the disease such as redness.
• Tear film break-up time (TFBUT). TFBUT can also illuminate a dry eye issue; the cut-off for dry eye diagnosis is less than five seconds.7
• Ocular protection index (OPI). The OPI was developed to quantify the interaction between blinking and the tear film––thus providing a framework to assess the effects of tear film instability associated with dry eye.8
• Interblink interval visual acuity decay (IVAD). Because the severity of dry eye signs and symptoms may relate to a patient’s interblink visual acuity, a disruption in visual function and tear film stability can be measured by clinical technologies such as the IVAD test.
The Treatment Options
Advances in contact lens technology have broken the barrier between dry eye sufferers and contact lenses. Soft contact lens materials, including omalficon A and etafilcon A, have higher oxygen permeability than previous-generation lenses, allowing the eye to “breathe” easily and the tear film to replenish more readily. One study showed that senofilcon A (Acuvue Oasys, Johnson & Johnson) is particularly effective in improving comfort over time in habitual lens wearers who are exposed to adverse environmental conditions.3 These lenses were also shown to enhance wettability and improve comfort, which can eventually lead to fewer dropouts.
Rewetting drops can also be used. Proactively selecting the optimal care products for your patient’s particular lenses can enhance performance and the overall wear experience, which ultimately can reduce dropouts.
Despite the number of treatment options available today, nothing is as successful as establishing a management strategy with your patients that works best for their individual needs. Emphasize frequent check-ups and maintain a clear line of communication for long-term contact lens-wearing success. Pre-emptively treat dry eye first and then follow with a contact lens prescription that works best for a patient’s condition. This will help minimize dropouts at your practice and make your patients much more comfortable in their lenses.
1. Scaffidi RC, Korb DR. Comparison of the efficacy of two lipid emulsion eyedrops in increasing tear film lipid layer thickness. Eye Contact Lens. 2007 Jan;33(1):38-44.
2. Rumpakis J. New data on contact lens dropouts: an international perspective. Rev Optom. 2010 Jan;147(1):37-42.
3. Ousler GW 3rd, Anderson RT, Osborn KE. The effect of senofilcon A contact lenses compared to habitual contact lenses on ocular discomfort during exposure to a controlled adverse environment. Curr Med Res Opin. 2008 Feb;24(2):335-41.
4. Foulks G. What is dry eye and what does it mean to the contact lens wearer? Eye Contact Lens. 2003;29:96-100.
5. Gonzalez-Meijome JM, Parafita MA, Yebra-Pimentel E, Almeida JB. Symptoms in a population of contact lens and noncontact lens wearers under different environmental conditions. Optom Vis Sci. 2007 Apr;84(4):296-302.
6. Walker PM, Lane KJ, Ousler GW 3rd, Abelson MB. Diurnal variation of visual function and the signs and symptoms of dry eye. Cornea. 2010 Jun;29(6):607-12.
7. Lemp MA, Hamill JR Jr. Factors affecting tear film breakup in normal eyes. Arch Ophthalmol. 1973 Feb;89(2):103-5.
8. Ousler GW 3rd, Hagberg KW, Schindelar M, et al. The Ocular Protection Index. Cornea. 2008 Jun;27(5):509-13.


