Conceptually, orthokeratology has been around for more than half a century now. But, it is the improvements in lens materials, design and fabrication over the last decade that have triggered significant changes in how we provide this treatment. When you consider the data published over that same 10-year span showed a retarding effect on the progression of myopia, it is clear that orthokeratology has never had greater potential to be a significant factor in the realm of vision correction––particularly for children.1-3 In this regard, it is an exciting time to be able to offer orthokeratology to our patients.
However, there still is much to study and learn about the long-term effects of orthokeratology on the corneal tissue. Reports of ocular infections with lens wear may cause patients to be nervous about pursuing orthokeratology, particularly when parents consider the procedure for their child. It is therefore important that we do our part to alleviate the concerns by knowing what risk factors exist and what problems may arise.
Why Ortho-K?
We can all agree that there are some indisputable benefits of orthokeratology—such as convenience and safety. Keep in mind that you should mention both the pros and cons of ortho-k with your patients.
First and foremost, we cannot understate the advantage of experiencing freedom from corrective lenses wear, especially for children. How many times have you had frustrated parents coming in for the fifth time in a month to get their child’s glasses fixed or adjusted? How often do children end up replacing glasses because they are broken or scratched to the point of uselessness? In general, children are harder on eyeglasses than adults—due to their active lifestyles and relative carelessness when it comes to their spectacles. Keep in mind that the long-term cost of orthokeratology vs. glasses is not significantly different when you consider that you are replacing glasses annually, if not more frequently.
Secondly, glasses are awkward to use when playing sports or other physical activities. This is one reason why many parents consider contact lenses in the first place. Many parents, however, are torn between concerns that their child is not ready for contact lenses and the alternative of their child having to wear glasses for athletics. Orthokeratology is a perfect solution for both of these problems. For children active in athletics, there is no better means of correction at any age than orthokeratology.
Ortho-K vs. Soft Contact Lenses
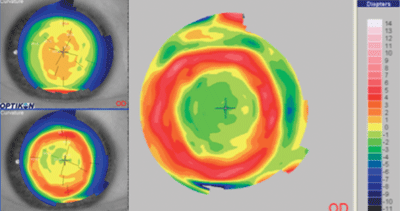
1. Pre- and post-treatment corneal maps, as well as a difference map for a child being corrected with orthokeratology lenses. Not only is the central cornea reduced in power, the mid-periphery is actually increased in power.
It could be debated that soft contact lenses can be just as advantageous for active children as orthokeratology, but the arguments fall short. For example, while soft lenses should not be worn when swimming, this is not an issue with orthokeratology.
Because soft lenses are worn during the active times of day, any problem with lens drying or stability will affect vision and function during times of visual demand. This is not the case with orthokeratology. Soft lenses are applied at home, but the child then spends the majority of their day away from home and, most likely, away from their care system, case and back-up glasses. This means that any issues that arise while wearing their soft lenses may not be managed optimally. On the other hand, with orthokeratology, children manage their lens use at home never far from assistance and lens care products.
Comparing cumulative costs, there is little monetary difference when you compare orthokeratology vs. soft lens use. Although the initial cost of orthokeratology is higher, the annual cost of soft lenses will usually catch up in the long run.
Myopia Control
One would-be advantage that is currently being researched is the possibility of myopia control through orthokeratology. One theory for why myopia progresses stipulates that the hyperopic defocus on the peripheral retina with standard forms of vision correction leads to further progression of myopia. With orthokeratology, only the central 4mm to 5mm of the visual axis is optimally corrected, while the peripheral retina is left in varying degrees of myopic defocus, as evidenced by looking at the topography of the cornea before and after treatment (figure 1). This myopic defocus leads to less development of myopia to a statistically significant degree.
Studies and published results indicate that slowing the progression of myopia is real with orthokeratology. In 2005, Pauline Cho, B.Optom., M.Ed., Ph.D., and colleagues published the first set of results that compared axial eye elongation in a group of children using orthokeratology lenses with a control group.1 Their research showed 46% less axial elongation in patients with ortho-k lenses vs. those in the contol group.1
In 2009, Jeffery Walline, O.D., Ph.D., reported nearly identical findings in a completely different patient population.2 These results have been followed with additional research in different areas of the world, including two 2011 studies—one by Tetsuhiko Kakita, M.D., and colleagues and one by Jacinto Santodomingo, Ph.D., M.Sc., and colleagues—which showed a slowing of axial elongation and vitreous chamber growth.3,4 Other tests are ongoing, including the Retardation of Myopia in Orthokeratology (ROMIO) Study, which is randomizing participants into orthokeratology or single-vision spectacles. Early results show data comparable to the other four previously mentioned studies.5
Evidence certainly is mounting to suggest that there is more to orthokeratology than just the obvious benefits of convenience—it may become increasingly clear that this option should be discussed with the parents of all children who are exhibiting myopia progression. At first, it may be difficult to get into the habit of discussing this treatment option––but, you will soon start to see the benefits of orthokeratology become a reality for your patients.
Minimizing the Risks

2. Using proper solutions and teaching proper technique are crucial to
minimizing the risk of complications for children in orthokeratology lenses.
If there are significant risks to ocular health with orthokeratology, the benefits may be negated. So, what are these risks? The main short-term concern is ocular infection, leading to loss of best-corrected visual acuity. Long-term risks revolve around morphologic change to the corneal tissue, which affect its function.
Ocular infection is a risk factor for any type of contact lens wear. Overnight lens wear is associated with a higher risk of ocular infection than daily wear lens use, but gas-permeable (GP) lens wear typically presents a lower risk than soft lenses.6
Additionally, how does the risk for keratitis compare in orthokeratology lens wearers to that of other lens wearers? The problem we face is that the volume of cases is relatively small to make a good estimation. We know that infectious keratitis does indeed occur, as several articles have chronicled these cases.7-10 The American Academy of Ophthalmology last published its stance on the safety of overnight orthokeratology in 2008, suggesting that a better-controlled, level 1 study needed to be completed to fully evaluate the risk and the potential for myopia control.11
What can we do in the meantime to minimize that risk to patients, specifically children? Clearly, good lens care practices are of the utmost importance (figure 2). Use of only approved contact lens care products, along with the elimination of tap water use on lenses, has been recommended to reduce the risk; the highest incidence of infectious keratitis occurs in regions of the world where good care practices are less likely to be followed.7
In addition, provide careful instruction to parents and children about what is to be expected with lens wear, and include comfort upon application, signs and symptoms of problems and after-hours contact information. These steps are vital to minimize the chance of a lens causing serious problems. Written directions and instructions, as well as informed consent, is highly recommended to all orthokeratology lens wearers.
Finally, using only high Dk/t lens materials and FDA-approved designs not only minimizes the risk to patients, but also improves the efficacy of the treatment.12 Requiring the highest level of compliance to accepted practices and the highest quality materials will minimize the risk of short-term complications for patients.
Long-term complications of orthokeratology involve permanent and undesirable changes to corneal shape or function. Some of these changes can be very significant, while others may not necessarily have any impact on ocular function. One study documented residual corneal flattening among a group of 28 patients; the impact of this change is still undetermined.13 Certainly, any change to the corneal tissue is bothersome, but mild flattening of the cornea may or may not create real issues. The aforementioned study evaluated keratometric change two weeks after discontinuation of lens wear vs. pre-treatment levels. It is possible that, with longer time out of lenses, the corneal curvature changes may return to baseline. But, it is also possible that some permanent stromal restructuring may occur.13
Reduction in corneal sensation has been documented after three months of overnight orthokeratology lens wear.14 The significance of this finding has not yet been determined, but it is useful to keep this in mind for our patients. Perhaps of more significance are the 2011 findings of Amelia Nieto-Bona, O.D., M.Sc., and colleagues, which examined the corneal tissue of 15 eyes with confocal microscopy. The researchers reported several changes to corneal tissue––some of which returned to baseline after discontinuation of lens wear, and others that showed an increase in endothelial cell polymegathism and a decrease in epithelial layer thickness.15 Again, the significance of these findings is not known, but studies continue to look at the possible long-term morphologic changes to the cornea as a result of orthokeratology and their effects on ocular health.
We all want what is best for our children. Good vision and ocular health are important aspects of our children’s lives. To be able to provide vision correction that is convenient, safe and effective at slowing the deterioration of their vision over time is something most of us would want for our children who require vision correction. Orthokeratology seems to be able to provide all these features. Further research will continue to determine the true short- and long-term safety for those children in orthokeratology lenses, as well as the effects it has on slowing the progression of myopia.
Dr. Jedlicka is the director of the Cornea and Contact Lens Institute of Minnesota, a referral practice dedicated to specialty contact lens fittings, contact lens research, and education to students and practitioners.
1. Cho P, Cheung, SW, Edwards M. The longitudinal orthokeratology research in children (LORIC) in Hong Kong: a pilot study on refractive changes and myopia control. Curr Eye Res. 2005 Jan;30(1):71-80.
2. Walline JJ, Jones LA, Sinnott LT. Corneal reshaping and myopia progression. Br J Ophthalmol. 2009 Sep;93(9):1181-5.
3. Kakita T, Hiraoka T, Oshika T. Influence of overnight orthokeratology on axial elongation in childhood myopia. Invest Ophthalmol Vis Sci. 2011 Apr 6;52(5):2170-4.
4. Santodomingo-Rubido J, Villa-Collar C, Gilmartin B, Gutiérrez-Ortega R. Myopia control with orthokeratology contact lenses in Spain (MCOS): study design and general baseline characteristics. J Optom. 2009;2(4):215-22.
5. Berntsen D. Orthokeratology and myopia control—what do we know? CL Spectrum. 2012 Feb; 27:14-5.
6. Stapleton F, Keay L, Edwards K, et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmology. 2008 Oct;115(10):1655-62.
7. Watt KG, Swarbrick HA. Trends in microbial keratitis associated with orthokeratology. Eye Contact Lens. 2007 Nov;33(6 Pt 2):373-7.
8. Chee EW, Li L, Tan D. Orthokeratology-related infectious keratitis: a case series. Eye Contact Lens. 2007 Sep;33(5):261-3.
9. Kim EC, Kim MS. Bilateral Acanthamoeba keratitis after orthokeratology. Cornea. 2009 Apr;28(3):348-50.
10. Shehadeh-Masha’our R, Segev F, et al. Orthokeratology associated microbial keratitis. Eur J Ophthalmol. 2009 Jan-Feb;19(1):133-6.
11. Van Meter WS, Musch DC, Jacobs DS, et al. Safety of overnight orthokeratology for myopia: a report by the American Academy of Ophthalmology. Ophthalmology. 2008 Dec;115(12):2301-13.
12. Lum E, Swarbrick HA. Lens Dk/t influences the clinical response in overnight orthokeratology. Optom Vis Sci. 2011 Apr;88(4):469-75.
13. Wu R, Stapleton F, Swarbrick HA. Residual corneal flattening after discontinuation of long-term orthokeratology lens wear in Asian children. Eye Contact Lens. 2009 Nov;35(6):333-7.
14. Hiraoka T, Kaji Y, Okamoto F, Oshika T. Corneal sensation after overnight orthokeratology. Cornea. 2009 Sep;28(8):891-5.


