With an estimated 4.91 million Americans over the age of 50 suffering from dry eye, eye care practitioners are perpetually on the lookout for better treatment options.1 What about scleral lenses? We commonly associate scleral lens fittings with corneal irregularities, since the lenses hold a liquid reservoir that allows them to mask the irregularity and return patients to near normal visual function. However, the liquid reservoir these lenses hold can also aid in effectively managing and providing relief for patients with dry eye. This article offers advice for using scleral lenses to treat moderate to severe dry eye.
Understanding Dry Eye
Evaporative dry eye has been strongly linked to meibomian gland dysfunction (MGD), whereas aqueous-deficient dry eye is often secondary to systemic disease—such as Sjögren’s syndrome and chronic graft vs. host disease (cGVHD).2
The best approach to managing dry eye is based upon its etiology and severity. Scleral lenses are typically reserved for helping to manage moderate to severe dry eye disease. In 2007, the International Dry Eye Workshop recommended that contact lenses be considered for Grade 3 level of severity.3 Grade 3 patients have chronic dry eye that affects their comfort and vision, which can potentially limit their activity. These patients often present with lid disease (figure 1), central corneal staining (figure 2), filamentary keratitis, mucus clumping and increased tear debris. This results in severe discomfort and decreased visual acuity.
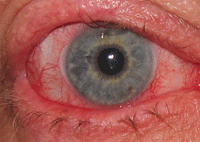
1. Severe lid disease in a patient with cGVHD.
Treating Dry Eye
Recent literature reports success in managing moderate to severe dry eye disease with scleral lenses. In 2012, researchers used mini-scleral contact lenses for moderate to severe dry eye patients previously unsuccessful in conventional therapy. They found that four of the seven patients fitted in scleral lenses reported reduced discomfort and dry eye symptoms, decreased use of artificial tears and improved visual acuity.4
A retrospective case series of five patients (10 eyes) who were successfully fit with Jupiter scleral lenses was analyzed in a 2008 study to better understand the use of scleral lenses in the management of chronic graft vs. host disease.5 All patients reported improved comfort, and seven of the 10 eyes demonstrated improved best-corrected visual acuity.
A 2007 study on the use of scleral lenses to manage severe dry eye related to cGVHD followed 33 patients with severe dry eye secondary to cGVHD and had previously failed conventional treatment. Study patients were fit with the Boston scleral lens prosthetic device (BSLPD); the results showed that management with the BSLPD produced an improvement in pain, photophobia and general quality of life for nearly all patients.6
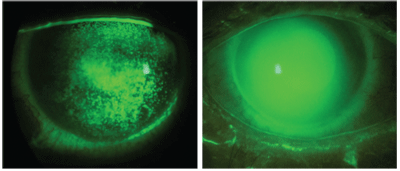
2,3. Corneal staining of a patient with cGVHD (left). A 18mm scleral fit for a patient with cGVHD (right).
Fitting Scleral Lenses
When fitting scleral lenses, the objective is to achieve complete lens clearance of the cornea, evenly distributed haptic bearing that doesn’t excessively compress the bulbar conjunctiva and a semi-seal fit. However, there are some special factors to consider when fitting a scleral lens specifically to manage dry eye.
• In dry eye patients, avoid using smaller corneo-scleral lenses (12.5mm to 15mm in diameter) because they are more likely to exhibit some shared bearing between the cornea and the sclera. It’s important that the scleral lens completely vaults the cornea to avoid mechanical injury, especially when the cornea is already compromised due to dryness. Mini-scleral lenses (15mm to 18mm) or full scleral lenses (18mm to 24mm) are a better choice for managing dry eye because they provide increased vaulting capability (figure 3).
Although the ideal vaulting range for mini-scleral or full scleral lenses varies between 100µm to 300µm, it’s best to err on the side of more vault to ensure that you have enough liquid reservoir across the entire cornea, including the limbus.
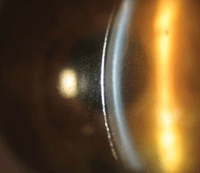
4. A scleral lens with significant reservoir debris.
• Inform your patients in advance that scleral lenses may require extra care due to possible complications. Patients who have moderate to severe dry eye produce significantly more mucus and usually exhibit excessive tear debris. Unfortunately this excessive debris gets pumped underneath the lens and builds up during wear time (figure 4). Reservoir debris does not diminish comfort, but it can negatively affect vision by causing the patient’s visual field to appear cloudy. In this case, a symptomatic patient will have to remove lenses for rinsing and refilling.
Your patients are less likely to be discouraged with scleral lens wear if they have been previously educated on these potential scenarios. Minimize the impact by fitting the haptic as evenly as possible to the scleral conjunctiva. Small areas of haptic edge lift can be an entrance port for debris, which can result in increased accumulation in the reservoir of the lens. Fitting the patient in a back surface toric or quadrant specific back surface design can minimize or eliminate edge lift.
Special Considerations
• Don’t forget about the eyelids. Chronic blepharitis or MGD can be a contributing factor for moderate or severe dry eye disease. Habitual use of lid scrubs and warm compresses can help improve the patient’s tear film. Consider oral or topical pharmaceuticals for severe lid disease or to treat patients who are unsuccessful with lid scrubs and warm compresses.
 • Pick the right solution. Prescribing the appropriate solution is an important step in successfully managing dry eye with scleral lenses. Have the patient use a hydrogen peroxide care system for cleaning and disinfection. This will ensure that no residual preservatives get trapped underneath the bowl, which could later become toxic to the anterior ocular surface. Prescribe the off-label use of 0.9% saline (single-use ampules to avoid toxic exposure to preservatives or buffers in bottled saline solutions). Consider having the patient use an extra-strength cleaner periodically if they are prone to deposits and build-up of debris.
• Pick the right solution. Prescribing the appropriate solution is an important step in successfully managing dry eye with scleral lenses. Have the patient use a hydrogen peroxide care system for cleaning and disinfection. This will ensure that no residual preservatives get trapped underneath the bowl, which could later become toxic to the anterior ocular surface. Prescribe the off-label use of 0.9% saline (single-use ampules to avoid toxic exposure to preservatives or buffers in bottled saline solutions). Consider having the patient use an extra-strength cleaner periodically if they are prone to deposits and build-up of debris.
• Redefine the role of eye drops. Patients referred for severe dry eye secondary to a systemic issue (e.g., cGVHD) will probably be on numerous topical medicines, including steroids, autologous serum and antibiotics. If the scleral lenses are successful, often the dosage can decreased or eliminated altogether. Comanage any medication changes with all other professionals involved in the patient’s care. The patient may continue to use artificial tears during lens wear to keep the surface lubricated; topical lubricating gels may be used at night after lens removal.
Moderate to severe dry eye is a disabling condition that can limit a patient’s activity and decrease their quality of life. The use of scleral lenses for dry eye patients who have been unsuccessful with conventional therapy can significantly improve comfort and vision.
Dr. DeNaeyer is the clinical director for Arena Eye Surgeons in Columbus, Ohio, and a consultant to Visionary Optics, Bausch + Lomb and Aciont. You can contact him at [email protected]. Dr. DeNaeyer is the designer of the Europa scleral lens (Visionary Optics).
1. The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007 Apr;5(2):93-107.
2. Nichols KK. The international workshop on meibomian gland dysfunction: introduction. Invest Ophthalmol Vis Sci. 2011 Mar 30;52(4):1917-21.
3. Management and therapy of dry eye disease: report of the Management and Therapy Subcommittee of the International Dry Eye Workshop (2007). Ocul Surf. 2007 Apr;5(2):163-78.
4. Alipour F, Kheirkhah A, Behrouz M. Use of mini-scleral contact lenses in moderate to severe dry eye. Cont Lens Anterior Eye. 2012 Dec;35(6):272-6.
5. Shornack M, Baratz KH, Patel SV, Maquire LJ. Jupiter scleral lenses in the management of chronic graft versus host disease. Eye Contact Lens. 2008 Nov;34(6):302-5.
6. Jacobs DS, Rosenthal P. Boston scleral lens prosthetic device for treatment of severe dry eye in chronic graft-versus-host disease. Cornea. 2007 Dec;26(10):1195-9.


